Peter Daszak has spent the past three decades attempting to predict global pandemics. He leads a group of international investigators who try to anticipate when and where outbreaks will happen and how far they will travel. “Pandemic prediction is a bit like earthquake prediction,” Daszak recently told me from his office in Manhattan. “There are lots of tremors, and occasionally you get a big one. Ebola was the big one.”
The Ebola outbreak caught us all off guard. As an infectious-disease physician who practices in Manhattan, I readily answered basic questions about the virus, but I got uncomfortable as soon as things got nuanced. Could it go airborne? I didn’t think so, but I wasn’t sure. And that’s because I wasn’t prepared for it. None of us was.
Any new health threat comes with uncertainties, which can be twisted into the suggestion that experts don’t really know what they’re doing. In the worst cases, this leads to panic or suspicion of medical advice. Part of preventing that scenario has to do with better communication and public relations. But a much larger part involves knowledge. Infectious-disease discovery must become a public health priority. We need to know what diseases are out there and which ones are coming for us; we need to be prepared.
Scientists estimate that between 1940 and 2004, 335 new infectious diseases appeared in humans. This number includes pathogens that likely entered our species for the first time, such as HIV, and newly evolved strains of familiar organisms, such as multidrug-resistant tuberculosis. The majority of these diseases—about 60 percent—were caused by zoonotic pathogens, meaning they were transmitted to humans from animals. And of those, about 70 percent were from animals that typically live in the wild. (Two of the last global pandemics—SARS and Ebola—were caused by viruses that appear to live in bats.) Interestingly, the percentage of human diseases coming from wild animals seems to be rising—and quickly. But why? And more importantly, what can we do about it?
Daszak is trying to give us answers. As president of the EcoHealth Alliance, he leads a team that has analyzed hundreds of new infectious agents, trying to determine the factors that allow a disease to make the leap from animal to human. His group does this by traveling to biodiversity hot spots—Bangladesh, Malaysia, Brazil—to sample wildlife known to harbor unstudied viruses. When team members discover one, they enlist mathematicians to run computer models to predict the likelihood of human transmission.

Daszak, right, at a free range poultry farm in China.
Photo courtesy of Peter Daszak
This type of investigation, referred to as mathematical epidemiology, has long been the basis for our understanding of how most pathogens emerge, evolve, and spread. But the nature of outbreak prediction is becoming more sophisticated, as Daszak and others have increasingly incorporated insights from behavioral economics to improve the quality of outbreak prediction and prevention.
Economic behavior plays a vital role in disease transmission. Trade affects the number of humans exposed to a pathogen, which means it’s possible to model a potential outbreak as a function of commerce. This approach, referred to as economic epidemiology, has recently opened up a new set of prediction tools and prevention strategies.
“We’ll tell a local government that there’s a market selling bats and we found a lethal virus in those bats,” Daszak told me. “You can shut down that market. There’s a rat breeder I know in Guilin, China, who sells them for food. We test his rats to make sure they’re safe to eat.”
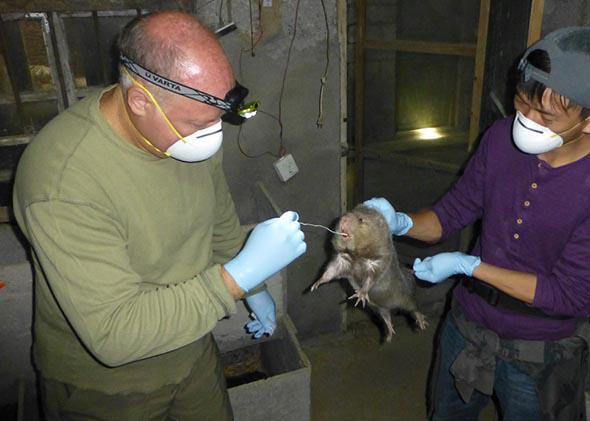
Daszak, left, at a rat farm in Guangxi Province, China.
Photo courtesy of Peter Daszak
Daszak’s team has identified three factors that help a virus take hold in people: human population density, wildlife diversity, and changes in land use. “The worst thing you can have,” he told me, “is a place where you have rapidly growing human population—West Africa, China, or India—in a place with a lot of wildlife diversity, like near a rain forest. It creates a pathway for a virus to go directly from animal to humans.”
There are believed to be about 320,000 viruses in the world that infect mammals (some estimates push that number even higher), and it’s been projected that it could cost about $6 billion to discover and characterize them. “In the next 20 years, we’ll find all of them,” Daszak said. “Then we’ll figure out which ones are the most likely to emerge as a global pandemic.” Given viruses’ high mutation rates and abilities to colonize new hosts, the next pandemic will likely be caused by a virus. Recently, two candidates have emerged: Nipah virus and Rift Valley fever.
Nipah was identified in 1999 after a cluster of Malaysian pig farmers developed encephalitis. (The virus is named after a village where an infected patient lived.) Farmers were developing a sudden onset of fever, headache, vomiting, and diffuse muscle aches; 60 percent were in a coma within one week of becoming infected and more than 70 percent died.
Infection occurred through direct contact with respiratory secretions and urine from infected pigs. More troublingly, there was also evidence that Nipah may have been transmitted from person to person—a Malaysian nurse who cared for infected patients was found to have the hallmark blood and brain abnormalities of the disease, despite the fact that she had no exposure to infected animals.
The disease has spread from Malaysia since then. “Every year, we see an outbreak of Nipah virus in Bangladesh,” Daszak said. “[Outbreaks are] small right now, but they’re extremely lethal. More lethal than Ebola, but less transmittable. But viruses evolve … they’re supreme evolutionary machines.”
The other candidate for a pandemic among humans, Rift Valley fever, was identified in 1931 during an epidemic among sheep on a farm in the Rift Valley of Kenya. Transmission to humans occurs via bites from infected mosquitoes or through close contact with infected mammals. Symptoms are similar to those of Ebola, including the acute onset of fever and headache, and hemorrhage from the gastrointestinal tract. The largest human outbreak of Rift Valley fever occurred during the rainy season in Kenya in 1997–1998, when nearly 90,000 people were infected and 478 died. Although not as lethal as Ebola or Nipah, it still worries epidemiologists. “Rift Valley fever is transmitted by mosquitoes,” Daszak said, “which means it can get on a plane—there’s an average of 1.2 mosquitoes on every flight—and that means it could spread quickly.”
The Ebola epidemic in West Africa isn’t over, but as it recedes from the headlines, it’s time to consider what’s coming for us next. Pandemic prediction isn’t cheap, but waiting for an outbreak to happen can be even more costly. Economic losses due to SARS were estimated to be anywhere from $15 billion to more than $50 billion; the cost of the Ebola outbreak will almost certainly exceed that figure. By contrast, Daszak estimates that it would cost a total of $6.3 billion to discover all of the viruses that infect mammals—a fraction of the cost required to respond to a global pandemic like Ebola or SARS—and that information will ultimately lead to better disease monitoring, treatment, and preventative measures at the cusp of the next outbreak. It’s a massive endeavor, but a necessary one. Once we know what’s out there, we’ll be able to figure out what’s coming for us.
