Thomas Eric Duncan first arrived at Texas Health Presbyterian Hospital on the night of Thursday, Sept. 25, with a fever, abdominal pain, dizziness, and nausea. What doctors failed to realize then is that Duncan had Ebola—the first case to be diagnosed in the United States. That was only the beginning of the hospital’s problems. In the three weeks since, Duncan has died and two nurses who cared for him became the first people to contract the deadly virus while on U.S. soil.
Saturday, Sept. 20: Thomas Eric Duncan arrives in Dallas.
The hospital isn’t the only one second-guessing its own reaction. The director of the U.S. Centers for Disease Control and Prevention, Thomas Frieden, expressed his own regret earlier this week that his agency had not done more to help control the infection. He said that the CDC will now dispatch rapid response teams to any U.S. hospital with a confirmed Ebola case. “I wish we had put a team like this on the ground the day the first patient was diagnosed,” Frieden said.
Many details about Duncan’s care remain unknown, unconfirmed, or in dispute. But here is our best attempt at a timeline based on information from Varga’s congressional testimony; Duncan’s medical records, which were obtained by the Associated Press; and a lengthy statement provided by National Nurses United, a union that is serving as the voice for an unknown number of Presbyterian Hospital nurses who have raised serious allegations of missteps, mistakes, and failures during Duncan’s treatment.

Photo by Stewart F. House/Getty Images
The 42-year-old is in the United States to see his family. He had previously been living alone in a small room he rented in the Liberian capital of Monrovia. Four days before boarding a plane for the United States, Duncan reportedly helped take his landlord’s pregnant and Ebola-stricken daughter to and from the hospital, the point at which he was likely exposed to the deadly virus. (Duncan’s nephew, Josephus Weeks, has since denied this detail, claiming that his uncle had told him that he hadn’t helped the pregnant woman.)
Wednesday, Sept. 24: Duncan begins to develop symptoms.

Photo by Dominique Faget/AFP/Getty Images
This is the first point at which Duncan would have been contagious.
Thursday, Sept. 25, approx. 10:30 p.m.: Duncan goes to the ER.

Photo by Joe Raedle/Getty Images
He arrives at the Texas Health Presbyterian Hospital emergency room with a fever of 100.1, abdominal pain, dizziness, nausea, and a headache. At some point during his ER stay, a nurse makes a note that Duncan had recently arrived from Africa—but that information never makes it to the attending physician, according to the AP. According to the hospital, Duncan was examined and underwent “numerous” tests over the next four hours. At one point, his temperature spikes to 103 before dropping to 101.2. Doctors ultimately conclude that his symptoms are “not severe.” Medical records provided to the AP, however, show that Duncan had reported experiencing “severe pain” and that at some point medical staff marked his 103-degree fever with an exclamation point on his chart.
Friday, Sept. 26, early morning: Duncan is discharged.
He is given a prescription of antibiotics and instructions to take Tylenol.
Sunday, Sept. 28: Duncan returns to the ER.
Duncan is rushed by ambulance back to the hospital. He is suffering from diarrhea, abdominal pain, nausea, and vomiting. This time his symptoms—and recent travel history—prompt staff to decide that he is an Ebola risk. The CDC is notified.
Sunday, Sept. 28 - Tuesday, Sept. 30: Conflicting accounts.
Much of what happens between when doctors first deem Duncan an Ebola risk and when a blood test confirms those suspicions remains in dispute. Among the areas of concern:

Photo by Stewart F. House/Getty Images
General protocol: According to Varga, the hospital “followed all CDC and Texas Department of State Health Services recommendations.” The nurses tell a different story. “There was no advance preparedness on what to do with the patient, there was no protocol, there was no system,” according to the union.
Isolation: The hospital has suggested that Duncan was quickly isolated from other patients. The nurses union, however, alleges that he remained around other patients for “several hours” and that an initial attempt by a nurse supervisor to have Duncan moved to an isolation unit was met with “resistance from other hospital authorities.”
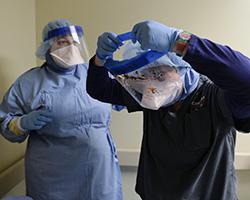
Photo by Cyrus McCrimmon/Denver Post via Getty Images
Protective gear: Nurses and doctors reportedly cared for Duncan while wearing standard hospital gowns instead of hazmat suits—a detail not refuted by Varga, who said only that staff wore “protective equipment” like “water impermeable gowns,” surgical masks, eye protection, and gloves. According to the nurses union, no one at the hospital knew “what kind of personal protective equipment should be worn,” and some nurses had to rely on medical tape to cover exposed body parts. It also remains unclear exactly when staff began wearing shoe covers—a step that should have been implemented immediately to prevent workers from tracking Duncan’s contagious body fluids around the hospital. According to medical records, at one point a doctor suggested shoe covers should be considered but appears to have stopped short of making them mandatory. Varga, meanwhile, says the shoe covers “were added shortly” after the initial protective gear.
Blood work: The nurses union claims that Duncan’s lab work was sent through the hospital’s pneumatic tube system without any special precautions, an action that risked contaminating the entire system.

Photo by Joe Raedle/Getty Images
Secondary isolation: According to the nurses union, hospital officials allowed nurses who had cared for Duncan to continue their normal patient rotations “even though they had not had the proper personal protective equipment” while caring for him. The union also alleges that patients who may have been exposed to Duncan were isolated for only a single day, even though any patient with a low-grade fever could have potentially been contagious.
Hospital officials say that as many as 76 staff members may have been exposed to Duncan before he died but have not said exactly how many treated him prior to his official Ebola diagnosis.
Monday, Sept. 29: Nina Pham treats Duncan for the first time.
Pham, a 26-year-old nurse, will later become the first person known to have contracted Ebola while in the United States. According to the AP, there is “no indication” in the records that Pham “donned any protective gear” during her first encounter with Duncan, although records show she did during her subsequent visits to his room.
Tuesday, Sept. 30: Positive test result.
The CDC confirms that Duncan has Ebola.
Wednesday, Oct. 8: Duncan dies.

Photo by Joe Raedle/Getty Images
His longtime partner, Louise Troh, and her 13-year-old son, meanwhile, remain quarantined in Dallas. “I am now dealing with the sorrow and anger that his son was not able to see him before he died,” Troh says in a statement, a reference to the 19-year-old son the couple had together, who was away at college when the hospital put his father in isolation. “This will take some time, but in the end, I believe in a merciful God.”
Friday, Oct. 10: Nurse travels to Ohio.
Amber Joy Vinson, a nurse who cared for Duncan and who will later become the second person known to have contracted Ebola in the United States, takes a commercial flight from Dallas to Cleveland to visit family in Akron, Ohio. She was showing no symptoms at this point but, according to the CDC, health workers who had treated Duncan had been advised to stay home and avoid public transportation. The CDC will later confirm, however, that Vinson was given the green light to fly to Ohio. It is unclear why.
Friday, Oct. 10: Pham shows symptoms.
Pham, who, medical records show, cared for Duncan on and off from the day after he was admitted to the day before he died, is placed in isolation in the Dallas hospital.
Sunday, Oct. 12: A second positive.

Photo by Mike Stone/Getty Images
The hospital confirms Pham’s positive test results for Ebola. Confusion reigns as the hospital first says it will divert all emergency room visits to other area hospitals, then says it won’t, before finally reverting to the original diversion plan.
Monday, Oct. 13: Vinson returns.
Vinson returns from Cleveland to Dallas–Fort Worth on Frontier Airlines Flight 1143 with 132 other passengers. She had a low-grade fever of 99 degrees—below the 100.5 threshold at which doctors believe a patient is contagious—and, the CDC says, she did not have any symptoms likely to have put others on the flight at risk. According to an agency spokesman, Vinson was cleared to make the trip back to Texas by a CDC official. Again, it is unclear why.
Tuesday, Oct. 14: Vinson admitted to the hospital.
Vinson arrives at Texas Health Presbyterian Hospital with a low-grade fever and is placed in isolation.
Wednesday, Oct. 15: A third positive, a first transfer.

Photo by Kevin C. Cox/Getty Images
Vinson becomes the third person to be officially diagnosed with Ebola in the United States. She is said to be “ill but clinically stable” and is later transferred by air ambulance to Atlanta’s Emory University Hospital, which has one of four biocontainment units in the country.
Thursday, Oct. 16: A second transfer.
Pham is to be transferred to the National Institutes of Health in Bethesda, Maryland, which also has a biocontainment unit. (The country’s other two biocontainment units are at University of Nebraska Medical Center and St. Patrick Hospital in Missoula, Montana.) In his testimony to Congress, Varga apologizes for the mistakes made at Texas Health Presbyterian Hospital.
