Excerpted from Extreme Medicine: How Exploration Transformed Medicine in the Twentieth Century by Kevin Fong, out now from The Penguin Press HC.
On Aug. 31, 1940, the Battle of Britain was reaching a critical phase when Hurricane pilot Tom Gleave’s aircraft came under enemy fire. In a few short seconds, the center of Gleave’s cockpit had become the head of a blowtorch. The aluminum sheet in which the dials of his control panel were set began to melt. Trapped with his plane ablaze and falling from the sky, Gleave’s hand fell to the butt of his service revolver and momentarily he considered a quicker, less painful end.
However, there was one last chance. If he could open the canopy, pitch the aircraft forward and flip it over onto its back, then perhaps the maneuver would fling him out. Gleave tore his flying helmet off, severing his last connections to the Hurricane. He slid the canopy open, shoved the control column forward, and then everything around him exploded.
He found himself propelled for many yards, enveloped in a ball of flames, finally breaking free into thin air and then tumbling toward the ground. Finding the D-ring of his ripcord, he pulled hard and felt the unfurling of his parachute and a comforting tug as its silk canopy inflated above him.
He hit the ground hard and fell onto his side, somehow managing to avoid further injury. Releasing his parachute, Gleave eventually found the strength to get to his feet. His boots and socks appeared to be intact and largely unburned. But that was where normality ended.
His trousers had gone except for a small patch protected by the parachute harness. Above his ankle, the skin over his right leg had blistered and ballooned along its whole length. His left leg was in much the same state, save for a patch of skin over his thigh, which had been relatively spared. The underside of his arms and elbows were burned, and the skin hung in charred folds from his hands and wrists.
His head and neck, too, had been exposed to the inferno, and his eyes were little more than slits. His nose had been all but destroyed. Somehow he staggered across the field toward a gate on its far side, shouting for help as he went. “RAF pilot,” he blurted out. “I want a doctor.”
You can just about bear to hang on to a mug of hot tea at 108 degrees. That’s just 10 degrees higher than your normal core body temperature. It’s pretty unimpressive, really, but that is where the limits of human endurance lie. The sensation that forces you to drop the cup is set in motion by a clever receptor: a weave of proteins in the dermis attached to an ion-channel control that opens or closes depending on how hot the channel is. The proteins convert the sensation of heat into pain.
The proteins that that receptor is built from, and those that stack together to build everything from your digestive tract to your DNA, start to fall apart at 113 degrees. That’s where the physiology of thermal injury starts. As temperatures climb, cells lose their capacity to self-repair; vessels begin to coagulate, tissues become irreversibly altered and later begin to die. All of this happens as you approach a temperature of around 140 degrees. Aircraft fuel, properly supplied with oxygen, can burn at over 1,800 degrees.
Tom Gleave woke underneath a bed in darkness. He was at Orpington General Hospital in the middle of an air raid; the bed was his makeshift shelter. He had survived, but the surgical teams at Orpington had little experience with such severe burns. The medical team at Orpington decided to transfer him to Ward 3 at the Queen Victoria Hospital in East Grinstead, which had developed a reputation for plastic reconstructive surgery under the leadership of Archibald McIndoe. Within resided a cadre of men disfigured by fire, and in 1940 the most severely injured of these were Hurricane pilots.
McIndoe came to Tom’s bedside and explained what needed to be done. It would take many months and dozens of surgeries, McIndoe explained. “You won’t like it,” he said, “but it’ll be worth it.”
Archie McIndoe was a New Zealander, originally invited to the United Kingdom to join the practice of his esteemed older cousin Harold Gillies, who had pioneered techniques of plastic surgery during the World War I, when a sailor burned at the Battle of Jutland was the first patient to undergo this type of surgery.
In retrospect, the cosmetic results of these surgeries look primitive at best. But at the time, the idea that badly damaged faces might be reconstructed in this way was revolutionary. It would fall to McIndoe to refine and advance these techniques, and the air war of the Battle of Britain would provide his defining challenge.
First, Gleave got new eyelids pinched from the unburned skin of his thighs. These tiny islands of skin were removed and sculpted into place. They were so small they could rapidly establish themselves at their new location on Gleave’s face, seizing upon the bed of vessels and perfused tissues that lay there waiting to be covered, like a minuscule sod of earth being transferred from one lawn to another. Oxygen and nutrients readily diffused into these small tokens of flesh. And the wounds left by taking these grafts were discrete enough that they could be left to heal spontaneously.
But larger patches can’t be moved in this way; their needs are more demanding. In plastic surgery, the battle, as Harold Gillies once put it, is between blood supply and beauty. A full-thickness flap of skin about the size of an adult’s palm, cut out and moved as a single slab, will die before it has a chance to pick up a new supply of blood.
To get around this problem, McIndoe would raise a flap of skin, leaving it attached at one edge like a trapdoor. This kept the flap alive, supplied by the vessels running through its attached edge, but left it fixed in position. McIndoe would then fold the sheet of skin into a tube, stitching its long edges to each other to protect its raw undersurface from infection.
To move this tube of skin, he would make an incision in the patient’s arm and form a pocket into which its free edge could be tucked. He would then stitch the flap into place, fastening arm to thigh in the process, and wait for it to heal into position. This healing could take weeks, during which the patient was handicapped by the strange new anatomical arrangement.
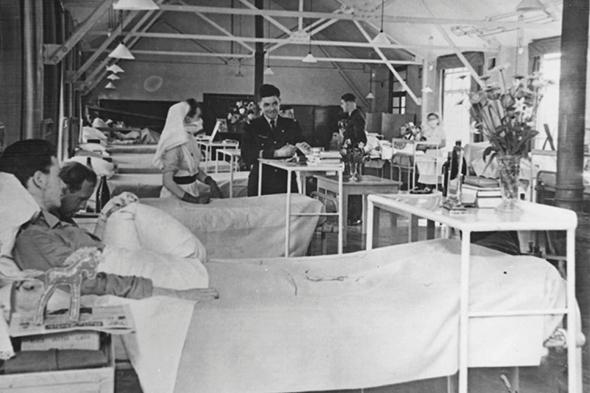
Photo courtesy of The Guinea Pig Club
Once the flap had established itself in the pocket, its link with the thigh could be severed. This arduous process left a flap of skin, previously from the thigh, now drawing its blood supply from the patient’s arm and free to be moved to any location which the arm could reach.
This process of walking a tube of skin end-over-end from one part of the body to another was known as waltzing. Gillies had invented the technique, but McIndoe brought it to maturity, waltzing flaps from larger areas than ever before. It provided the plasticity in McIndoe’s reconstructive technique, allowing him to address larger areas of burn injury by walking skin up from distant uninjured sites.
But aesthetic considerations were at the heart of McIndoe’s work. It was not enough simply to provide protective coverage; cosmesis was essential. Skin is indeed one of the principal organs through which we are able to experience the world. But McIndoe understood that it is also the means through which the world experiences us. When the war started and the toll of burned airmen began to become apparent, it was thought that the best thing you could do with the victims was to institutionalize them away from society with the intention of protecting one from the other. But McIndoe was unwilling to accept this fate for his patients, and his efforts in reconstructing the injured went far beyond surgical innovation. McIndoe would give them new faces, but they in turn would be expected to face the world again.
Ward 3 became famous for its feats of plastic reconstruction and notorious for the antics of its resident airmen. McIndoe resisted the militarization of the ward. The Queen Victoria Hospital was his—quite literally. The Air Ministry had seen that control of the facility was signed over to McIndoe, and it was run by his rules. Military discipline was relaxed, and rank ceased to have significance among the men in the beds—except, of course, when it came to McIndoe, whom they referred to as the Maestro, the Boss, or simply Sir. Beer kegs stood freely accessible on the ward, and at times it came to resemble something like a workingmen’s club.
All of this did something to distract from the grimness of the pilots’ reality. Not only were they assaulted by disturbing odors of char and infection, but they were also exposed to a series of strange new procedures that left them with arms stitched temporarily to thighs, abdomens, and faces, initially leaving them looking more bizarre than even their injuries had.
Confronted with long drawn-out weeks of suffering, with free beer as their only real comfort, the patients of Ward 3 set up a drinking club. At first they stumbled with the name, coming up with the Maxillonians, in reference to their ongoing maxillofacial surgeries. But they quickly realized that this was unwieldy and didn’t quite capture the spirit of their circumstances. They were a new breed of casualty patient under the care of a pioneer surgeon armed with groundbreaking techniques. They knew at heart that they were the subjects of experimentation—however well intentioned. And so the drinking party reformed under a new name: the Guinea Pig Club, with Tom Gleave the chief guinea pig.
The club’s activities moved rapidly beyond drinking and singing around pianos to rehabilitation and support. McIndoe orchestrated trips to East Grinstead. There the soldiers were dispatched, often under protest, to mix with the local population. The people of East Grinstead grew to embrace McIndoe and his army of strangely reconstructed men. They would make every effort to accommodate them, removing mirrors from their pubs, cafés, and restaurants and taking care to give the lives of McIndoe’s Guinea Pigs a veneer of normality. In time East Grinstead became “the town that never stared,” and it served as the perfect preparation for the Guinea Pigs’ reentry into a world that inevitably would.
Gallows humor became de rigueur for the Guinea Pigs. They recruited a treasurer with badly burned legs, so that he wouldn’t run off with the petty cash, and a secretary whose fingers had been injured, so he couldn’t keep minutes. At the start of World War II, the Guinea Pig Club was tiny. But with the onset of the bombing campaign, those numbers rapidly swelled, and by the end, its membership numbered more than six hundred. They were testing times that saw McIndoe and his team forced to refine their techniques as they went, learning from successes as well as mistakes. But these lessons would transform the field of plastic surgery.
The practice of military medicine during the war focused principally upon the salvage of life and limb. McIndoe didn’t save the lives of the Guinea Pigs, at least not immediately. That task was achieved by the hospitals that received them. But McIndoe’s work and the experience of those he treated taught clinicians that there was something at least as precious as life that modern medicine might preserve.
Excerpted from Extreme Medicine: How Exploration Transformed Medicine in the Twentieth Century by Kevin Fong, M.D. Reprinted by arrangement with The Penguin Press, a member of Penguin Group (USA) LLC, A Penguin Random House Company. Copyright © Kevin Fong, 2014.
