Along Interstate 55 in southern Missouri, farmland is dotted with for-sale signs, and billboards proclaim the area’s conservative politics. One says, “Vote for Life.” Another says, “Vote for anyone but Obama.” Dead armadillos litter the shoulder of the interstate. They are not native to Missouri, but as temperatures warm, they make their way up I-55, as do members of Colombian drug cartels. One of the highway’s final exits in southern Missouri is Cape Girardeau, population 40,000, an area of rural poor who suffer among the worst health outcomes in the United States.
This is where genetic counselor Melanie Baxter found herself a little more than a year ago, at St. Francis Medical Center. She specializes in cancer and found an immediate need there for her services; she helps patients to understand the results of genetic tests and to make treatment decisions for themselves and their family members. She’d been a genetic counselor at Siteman Cancer Center, part of Washington University School of Medicine in St. Louis. At Siteman, Baxter’s services were folded into the cost of the medical geneticist, who was always part of the patient care team. In Cape Girardeau, for the first time, Baxter had to worry about whether patients would get access to her care. At Siteman, if someone had asked Baxter how much her services cost, she couldn’t have answered. At St. Francis, she wondered how she was going to charge at all.
Office visits with genetic counselors can take several hours, and sometimes insurance companies won’t cover the time. At first, Baxter charged nothing. That lasted two weeks. Hospital administrators asked her to charge something, and they settled on $75 dollars, cash or check, payable at the time of the visit. That policy was in place for five months, and more than half of her patients said they couldn’t afford the fee, especially those who’d just been diagnosed with cancer and were already getting chemotherapy and radiation and had to pay for gas to travel to and from treatment. Eventually the hospital allocated charity money from its foundation to cover patients unable to afford the fee.
In the 21st century we have tremendous amounts of genetic data and analysis, and those data are used in medicine every day. But only some people can have access to or do anything with this knowledge. There is a patchwork of coverage across the United States. Depending on which state someone lives in, a genetic predisposition for cancer can either be a death sentence or a guide to proper preventive care. Obamacare may or may not fix this situation. The Affordable Care Act does cover genetic testing and should make tests less expensive for some people. The act also mandates that no coinsurance (cost sharing) can be charged for genetic tests. But coverage of follow-up counseling and care will still be determined by individual insurance providers. For people on Medicaid, state officials will determine coverage. Insurance coverage should not determine whether a person gets tested and treated. Access to genetic information is a matter of social justice. Preventing cancer is a matter of life or death.
Missouri typifies the genetic counseling situation in many states across the nation. While Missouri pays for genetic testing through its state-run Medicaid program, follow-up counseling care is covered on a case-by-case basis. Genetic counselors say they rarely win a case. These disparities hit women hard. The BRCA1 and BRCA2 tests for hereditary breast and ovarian cancers are the most common tests ordered by genetic counselors specializing in cancer. In many states, women on Medicaid find themselves in a particular treatment bind. A positive result on a genetic test is not considered a diagnosis in Missouri, so women play a risky game of “watchful waiting.”
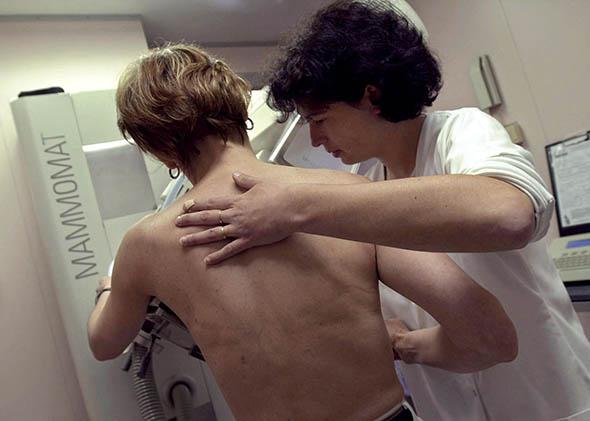
Women with certain BRCA mutations tend to get cancer young, before age 40. The lifetime risk can be as high as 90 percent. Women with a family history of breast or ovarian cancer are often advised to get tested for these mutations, especially if a family member has one of the mutations. A positive test result is the beginning of the story, not the end. Genetic counselors then need to help arrange follow-up care and find and test other family members who carry the same mutation. The medical recommendations for BRCA-positive women go way beyond “eat more fruits and vegetables.” To reduce the risk of breast or ovarian cancer, women may undergo bilateral mastectomies (as Angelina Jolie did), removal of ovaries before age 35 or when they’re finished having children, imaging every six months with either an MRI or a mammogram, chemoprevention with drugs that inhibit estrogen, or some combination of these treatments.
Although these treatments don’t bring the risk to zero, they can decrease the risk of both breast and ovarian cancer by more than 90 percent. Not all women may choose surgery, but women with good health insurance have a choice. Preventive surgery is not mandated. And if people have, say, a $5,000 deductible and a marginal income, genetic counselors will be back where they are now.
Here’s another gap in Obamacare: It does not require coverage of testing for people who already have cancer. That brings two problems. If people who are diagnosed with cancer subsequently test positive for a cancer-causing mutation, that information can guide which tests to order for family members without cancer who may also be at risk. Also, women diagnosed with breast cancer may be at high risk for ovarian cancer and not know it without a genetic test. The advocacy organization FORCE (Facing Our Risk of Cancer Empowered) has been lobbying the U.S. Preventive Services Task Force (which ACA guidelines are based on) to get this policy changed.
Even in a state like Massachusetts, which has had mandated health care for many years, genetic counselors still worry about bridging treatment gaps for those in need. Kristen Shannon, a genetic counselor at Massachusetts General Hospital Cancer Center, has to scramble to find preventive care for some of her patients depending on their insurance. “We run around like chickens to fill in the holes,” she says. At MGH, it’s always possible to get care, but she says it takes a lot of creativity and ingenuity on behalf of the genetic counselor and a significant amount of time. She worries about patients who are tested at health centers where counselors or physicians who order tests directly are not as well versed at finding help.
Women in Michigan are lucky. There, Medicaid covers both genetic testing and the follow-up care. A woman who tests positive for a cancer-causing mutation is covered for risk-reducing surgery, imaging, or chemoprevention, whichever she chooses, although she would need prior authorization for the surgery. “We look at this as medically necessary standard of care, and have offered this type of coverage for a long time,” says Debbie Eggleston, chief medical consultant for Michigan Medicaid. Eggleston says her team is hoping a number of women will be eligible under Healthy Michigan Coverage when it begins in April 2014. The plan will cover uninsured individuals who make less than 133 percent of the federal poverty limit.
Suzanne Mahon, a genetic counselor at Saint Louis University, a Catholic institution in midtown St. Louis, runs a program that turns no one away. She writes grants to the Susan B. Komen foundation to cover her salary and seeks other grants and donations to fund patients in need. She finds ways to get mammograms and MRIs and enlist surgeons. The effort is so time-consuming that Mahon published a study in the Clinical Journal of Oncology Nursing a few months ago detailing how much time she spent on every task for one year. The actual time she spends with patients and their families is 41 percent.
For Mahon, it’s unethical to test for BRCA mutations unless she can offer follow-up care. She sees the cost of a bilateral mastectomy as a given. “People should realize that it’s far cheaper to do prophylactic surgery than it is to wait for a cancer diagnosis and then do that surgery anyway, along with treatment such as radiation or chemotherapy, which is far more damaging to the body, and which is the very thing genetic counselors work to prevent,” she says.
Money can be a touchy subject for Mahon’s patients. She tries to help them understand that if they test positive for a BRCA mutation, getting preventive services will be difficult but not impossible, and the process will probably be demeaning. This is a hard conversation to have, and Mahon says she’ll repeat her main points over and over during a visit but isn’t always sure the women process what she tells them. Mahon has helped nine such women this year.
“All care is not created equal,” she says. “It should be but it’s not.”
Reporting for this story was supported by a fellowship from the Association of Health Care Journalists, with assistance from the Commonwealth Fund.