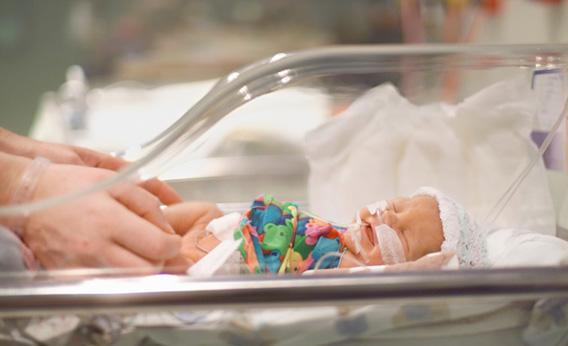
Twenty-two weeks into my pregnancy, my husband and I sat in one of the exam rooms at Mass General Hospital in Boston, talking with my ob about the possibility of a delivery in the next few weeks.
An ultrasound had showed that my baby was too small for the stage of my pregnancy and that levels of amniotic fluid were low, likely because of a deteriorating placenta that would soon fail. But according to the “preemie calculator” on the National Institutes of Health website, which I had been checking for several days, most babies as small as mine, born before 26 weeks, either die in neonatal intensive care, or survive with a moderate to severe impairment as a result of their prematurity. Reading Internet message boards, I had come across an alternative, one that seemed to be publicly discussed only in the safety of those anonymous forums: to do nothing and let the fetus miscarry.
I did not know if this would be ethical, even legal, but I told my doctor that I thought our priority was the baby’s quality of life. He got it, nodded, and asked me to name a target birth weight and gestational age after which I would choose to deliver rather than lose the pregnancy.
As my husband and I went home to come up with those numbers, I puzzled over the ethics of the situation. It seemed clear that our target age for delivery would be beyond 24 weeks, the point of viability after which a baby has a better chance than not of surviving outside the womb. Following the idea in Roe v. Wade that the states may pass antiabortion legislation to protect viable fetuses, I wondered if it would be right for me to let my pregnancy miscarry after the stage at which it would be illegal to terminate it, 24 weeks in Massachusetts. And yet, as my ob’s obvious past experience counseling parents in our situation suggested, my husband and I were far from alone in being asked to choose between a likely stillbirth—the name commonly used for a miscarriage after 20 weeks—and the risks of a very early delivery.
The proportion of pregnant women classified as “high-risk” in the U.S. today is rising, with government data showing that risk factors like diabetes and hypertension in pregnancy are becoming more prevalent and reports documenting advancing maternal age and growing numbers of multiple gestations as a result of fertility treatments. Many American women deliver before 37 weeks (defined by a group of obstetricians in Europe in 1970 as “term” for a human pregnancy, though the most common length is 40 weeks) without having any choice in the matter; they find themselves in preterm labor, or they develop life-threatening complications such as HELLP syndrome, for which delivery is the only cure. But other women are faced with a choice about whether to bring their babies into the world early. For example, of the tens of thousands of American women who carry twins every year, one in four pregnancies is diagnosed with the same problem of intrauterine growth restriction or IUGR, as my baby was, and so are at an increased risk of stillbirth.
This rising tide of high-risk moms comes as improvements in neo-natal technology have made it possible for babies to survive outside the womb at 22 or even—it has been reported—21 weeks. That means delivery is on the table as a potential option for a fetus at risk many weeks earlier than would have been the case a generation ago. Yet at the same time, there is a growing awareness of the long-term consequences of prematurity for babies.
Ahmet Baschat, a maternal-fetal medicine expert at the University of Maryland Medical Center who has researched outcomes in IUGR pregnancies, published a paper in 2007 in which he found that the proportion of IUGR babies who survived without experiencing serious complications of prematurity in the NICU reaches only 50 percent at 28 weeks, and is just under 90 percent at 32. “Nonintervention is always an option,” he says.
In some parts of the country, however, that option is rarely taken. Michelle Owens is a maternal-fetal medicine specialist at the Wiser Hospital for Women and Infants in Jackson, Miss. Most of her patients deliver before 34 weeks, for several reasons. First, Owens’ hospital has the state’s only Level 4 NICU, so women who are at risk of very early delivery tend to be referred there. Second, Mississippi has a high proportion of poor and uninsured women with chronic health problems like diabetes and hypertension that are not well controlled in their pregnancies and a large population of African-Americans who are prone to preterm birth. (The state’s preterm birth rate is 18 percent, compared with just under 12 percent for the nation as a whole.) Third, the hospital sees a higher proportion of religious women who are less likely to terminate a fetus with genetic abnormalities, some of whom are also at increased risk of delivering early. Owens says her hospital offers delivery for fetal distress after 23 weeks and that among her patients, choosing to take a high risk of stillbirth is “highly uncommon,” even for a baby estimated to have less than a 10 percent chance of survival on the outside. “Most of our moms want to give a 450 gram baby that is at the limit of what our NICU can do a chance,” she says. “They don’t want an in-utero demise.”
But I wasn’t so sure I felt the same way. And I may not be alone. After rising alarmingly for more than a decade, figures released in October by the National Center for Health Statistics reveal that the preterm birth rate has now fallen consistently for five years, from 2006 until 2011. This reduction is in large part due to obstetricians’ increasing caution about early delivery—in particular, many hospitals and health care systems have introduced programs to try to delay deliveries that were being scheduled between 34 and 36 weeks to 37 weeks or later, unless the timing is medically warranted. (Early term deliveries, at 37 or 38 weeks, are also being delayed to 39 weeks if possible.)
Of course, the intent of these programs is to delay deliveries without increasing the incidence of stillbirth. Still, Claudia Gyamfi, a maternal-fetal medicine specialist at New York-Presbyterian Hospital/Columbia University Medical Center in New York City, has noticed more caution among obstetricians about delivering early over the past four or five years, even at earlier gestations when there is a medical indication to do so. One option that OBs might offer to a woman whose fetus is at risk but who is reluctant to deliver too early is to begin fetal monitoring only after a gestation is reached when she would feel comfortable delivering, usually 28 weeks. “That’s patient autonomy,” Gyamfi says.
And what factors might play into that autonomy? With the preterm birth rate having peaked above 12 percent in 2006, more Americans today know family or friends raising preemies and are aware of the challenges those children can face even when they are not disabled: developmental delays, learning difficulties, behavioral problems, and other health issues. This firsthand knowledge changes the decision-making calculus for many women and couples. Just visit sites such as Inspire and BabyCenter to see the grueling consideration of options that many pregnant women go through.
On Inspire in 2011, for example, one Australian woman posted to say that she was 21 weeks pregnant and bleeding heavily. The end-diastolic blood flow through the umbilical cord had also reversed—a sign that fetal demise was imminent. She had been told there was no hope for her baby, a boy, and wanted to know from others if that was really true. She went on to say that she had been asking her doctor about delivery and photocopying information about miracle babies weighing only 300 grams who had survived. But, she added, she knew that her son would have to reach 500 grams to have a chance on the outside. (Her baby’s estimated weight was only just upward of 200 grams, though such estimates can be some ways off.) Other women, many based in the U.S., chimed in, holding out hope that she could be admitted and deliver in the next few days or weeks, but one Florida mother warned against a very early delivery, saying that while technology saves many babies, it can never imitate the womb, and that when a baby is very tiny and young, it can be better to let nature take its course. A couple of days later, the original poster reported that her baby had passed inside her.
Struck by the warning, I contacted the Florida mother, who, after being diagnosed with IUGR and preeclampsia, had delivered a little boy weighing a little over 600 grams at 26 weeks a couple of years ago. During a four=month NICU stay, her son was on a ventilator, underwent heart surgery, and suffered extensive damage to his lungs and brain. Ultimately, she and her partner made the decision to withdraw life support. She writes on Inspire that she didn’t realize she had the choice to wait longer before delivery but now does. (This isn’t to say that had she waited, she and her baby would have been fine.)
Despite these poignant online discussions, the ethics of very early delivery dilemmas mostly aren’t discussed publicly offline. “Assessing risks of stillbirth is a private decision, but so devastating to the individual families that they don’t tend to talk about it much,” Roger Young, an obstetrician at Fletcher-Allen Hospital in Burlington, Vt., told me. It’s easy to confirm that women regard such details as private. Inspire’s preemie board has recently seen a lot of discussion about privacy settings and the possibility of information posted there under screen names getting inadvertently linked into Facebook or Twitter where friends or family that aren’t supposed to know will see it. When I contacted women who had described online their experiences risking or opting for stillbirths to request interviews, most did not respond, and one removed some of her online material the next day. (As a result, I’ve only included case details that I feel are necessary to describe the issue.) Young says instances of women allowing a late-stage fetal demise, as I was considering doing, only rise to public attention when hospital staff disagree with the decision and get a court order to force a delivery. That happened most famously in the 1987 case of Angela Carder, a pregnant woman discovered to have terminal lung cancer who at 25 weeks did not consent to a C-section intended to prevent her fetus from dying with her. A court granted the hospital permission to operate, but after the baby and Carder both died, an appeals court vacated the ruling, leading to a legal precedent that a woman may not be forcibly delivered.
Still, the likelihood that something is legally permissible doesn’t make it ethical, or the right choice for an individual woman, and so I kept puzzling. My ob indicated that at Mass General, doctors would usually not recommend intervening on behalf of a fetus in our situation until 26 weeks, but that for our priorities, a suggested target might be 28 weeks and a birth weight of 750 grams. My husband and I were inclined to later targets—myself 30 weeks, he 32. But making it that far along, we were warned, was a long shot. My ob guessed that our baby had maybe a 25 percent chance of surviving to 28 weeks, but when pushed by my husband for a probability of making it to 32, wordlessly shook his head. Given the severity of our baby’s IUGR—she was at the third percentile, meaning that she was smaller than 97 percent of all fetuses, and the slowdown in her growth had begun already by week 18—the doctors expected that by 26 weeks, the amniotic fluid around her would be gone, and the end-diastolic blood flow in the umbilical cord would be absent or have reversed, halting growth and leading to signs of fetal distress such as heart-rate decelerations. It would be possible, my ob said, to monitor me closely over the next few weeks and follow that decline, delivering when reversed flow or fetal distress was seen.
I went with a different plan, along the lines outlined by Gyamfi, going without close or even weekly monitoring until after 30 weeks, my original delivery target. In the meantime, believing the prognosis, I started making practical arrangements for the stillbirth, which in Massachusetts would be recognized with a death certificate after 24 weeks. And yet, my baby kept kicking. When I went in for an ultrasound at 28 weeks, I was told that her weight was still less than even the ob’s suggested target of 750 grams, but that contrary to expectations there had been some growth, the fluid levels had recovered, and the blood flow through the cord, fetal movements, and heartbeat looked fine. The ultrasound doctor said something like, “It’s like you were 10 points behind in the first quarter and now you’re level in the second. It’s a totally different ball game.” My ob said that it was now more likely than not that there would be a live baby—even given our targets. On the way home in the car, my husband and I restarted a discussion we had suspended months earlier, about names.
There’s no sugar-coating a decision to wait. For all the cases in which it turns out the doctors have been overly pessimistic, there are many others with tragic outcomes. One woman who did respond to an interview request about losing her baby was an Ohio schoolteacher whose son Elijah had IUGR and was stillborn in 2011. (Update, Oct. 30, 2015: Due to the nature of the topic, we have removed the name of this woman at her request.) When reversed end-diastolic flow was first seen by ultrasound, the woman says she was offered an induction of labor, even though the baby was too small to have a chance of survival, the idea being that if she delivered, she might meet him alive, and that comfort care could be offered until he died.She decided against that option, both because she felt it would be more painful for him than passing on the inside, and because of her hope, unlikely as she understood it was, that he might not miscarry as predicted and survive to an estimated size of more than 450 gram, her delivery target. She went for regular ultrasounds to check on him until 26 weeks, when no heartbeat showed on the scan, and she was admitted to have him born still. “As horrible as it was, I still think we made the best of it,” she says.
My story has a very different ending. I hit my 30 week goal and then was monitored weekly, and then biweekly for fetal distress. By 33 weeks, none had shown, but I noticed a period of reduced fetal movement, and ultrasound showed that my baby now measured down below the first percentile (meaning, she was smaller than 99 percent of fetuses of that gestation). In the office appointment, my ob put the case for delivery urgently, and when I agreed, handed me paperwork for a C-section that he had already scheduled before the conversation to save time. Our daughter was born at 34 weeks, breathed on her own, and was transferred to a special-care nursery for five weeks to gain weight. Because of her breathing and relatively advanced gestation, she did not need to be admitted to the NICU. Five months later, she is an amazingly happy baby who is doing well at home.
This past June, a mother in Pennsylvania who had already lost a preemie baby after an early delivery and who was developing similar complications the second time around asked on Inspire whether women who had delivered early would in the future choose to deliver at 24 weeks when faced with an imminent stillbirth. Dozens weighed in, and, on balance, the mothers who had delivered early themselves expressed respect for women who opted to wait. One of the responses was from a California woman who had been waiting out an expected stillbirth from IUGR when she went into labor at 27 weeks and unexpectedly had her baby alive; she said whatever choice the woman makes is the best decision for her family.
To rest the question there, on a woman’s right to choose, may sound like an iteration of the abortion debate, but there are important differences, as I came to realize. Unlike a termination, neither a choice to deliver nor a choice to miscarry has a definite outcome, so women are dependent on counseling from their doctors to understand evidence or medical nuances that might tip them one way or the other. Given uncertainty, many obstetricians counsel in favor of delivery because—as Dr. Jay Iams of Ohio State University Medical Center says—stillbirth is the one option that isn’t treatable. Still, several experts I spoke to said that evidence-based guidelines for obstetricians who discuss stillbirth as a valid alternative to an early delivery would help women make more informed choices and standardize practice across the country, as might more public awareness of the existence of early-delivery dilemmas. I made my decision to take that very high risk of stillbirth on the information available to me at the time, without knowing how things would turn out. Some situations don’t present any right choices, but at least for me, interrupting a pregnancy with a delivery so early that my baby was not very likely to have a good outcome would have been the wrong one.